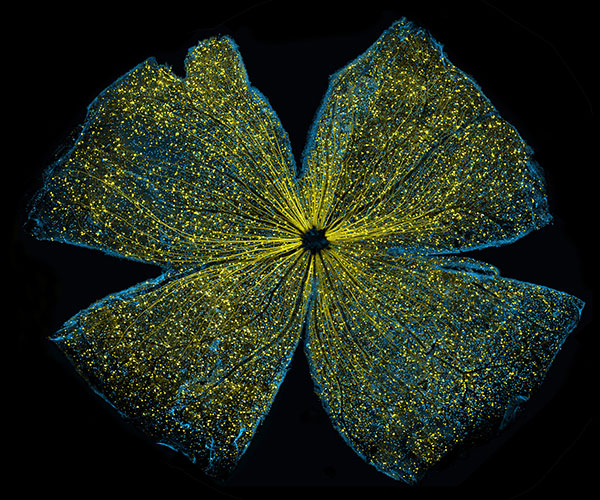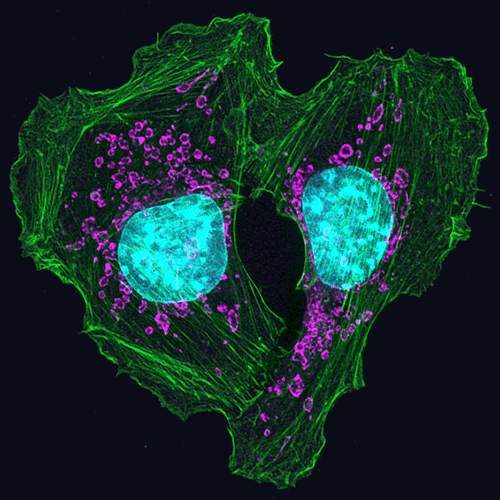
This heart-shaped image shows two mouse skin cancer cells connected to each other with actin, a protein that is part of the cellular skeleton. Researchers use mouse cells like these to tease out the molecular methods that cancer uses to invade new tissues in the body. It turns out that actin plays an essential role.
Cells can move as a collective, or independently. Movement of an individual cell requires a series of carefully controlled steps. Among them, a cell must break contacts with its neighbor cells and change its connections to the proteins and fibers around it. In addition, it must sense and follow a chemical path through the tissue it lies in. To do this, a cell changes shape, molding its membrane into flaps or feet called protrusions reaching in the direction it is traveling. Actin, among a variety of other molecules, is involved in all of these steps, but especially the shape change, when it gathers inside the cell membrane to help form the protrusions. Continue reading “Actin’s Many Roles”