Scientists may screen billions of chemical compounds before uncovering the few that effectively treat a disease. But identifying compounds that work is just the first step toward developing a new therapy. Scientists then have to determine exactly how those compounds function.
Different cancer therapies attack cancer cells in distinct ways. For example, some drugs kill cancer cells by causing their outer membranes to rapidly rupture in a process known as necrosis. Others cause more subtle changes to cell membranes, which result in a type of programmed cell death known as apoptosis.
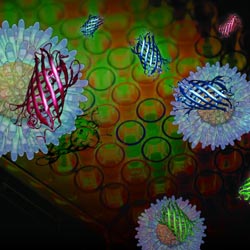
If researchers could distinguish the membrane alterations of chemically treated cancer cells, they could quickly determine how that chemical compound brings about the cells’ death. A new sensor developed by a research team led by Vincent Rotello of the University of Massachusetts Amherst can make these distinctions in minutes.
Continue reading “A Bright New Method for Rapidly Screening Cancer Drugs”