RNA is essential for life as we know it. Among other roles, this molecule helps translate the instructions of DNA into proteins, which perform a vast range of tasks to keep us alive and healthy. In past Biomedical Beat posts, we’ve discussed the basics of RNA and how researchers are using it to develop medicines, vaccines, and tests for certain diseases. This year, in honor of RNA Day on August 1, we’ve created a quiz all about this remarkable molecule. Test your knowledge with the questions below!
Continue reading “Quiz: Can You Solve These RNA Riddles?”Tag: COVID-19
Investigating Bacteria’s CRISPR Defense System to Improve Human Health

The earliest Andrew Santiago-Frangos, Ph.D., remembers being interested in science was when he was about 8 years old. He was home sick and became engrossed in a children’s book that explained how some bacteria and viruses cause illness. To this day, his curiosity about bacteria persists, and he’s making discoveries about CRISPR—a system that helps bacteria defend against viruses—as a postdoctoral researcher and NIGMS-funded Maximizing Opportunities for Scientific and Academic Independent Careers (MOSAIC) scholar at Montana State University (MSU) in Bozeman.
Becoming a Biologist
Although Dr. Santiago-Frangos wanted to become a scientist from a young age and always found biology interesting, by the time he was attending high school in his native country of Cyprus, he had developed a passion for physics and thought he’d pursue a career in that field. However, working at a biotechnology company for a summer changed his mind. “That experience made me want to dive into biology more deeply because I could see how it could be directly applied to human health. Physics can also be applied to human health, but, at least at that time, biology seemed to me like a more direct way to help humanity,” says Dr. Santiago-Frangos.
Continue reading “Investigating Bacteria’s CRISPR Defense System to Improve Human Health”Five Outstanding Stories From 2022
Throughout 2022, we shared the stories of dozens of NIGMS-supported researchers, trainees, and programs. We also highlighted new STEM education resources, tested your knowledge with quizzes, showcased extraordinary scientific images, and more. To celebrate the upcoming new year, we’re highlighting five of our most popular posts from 2022. Check out the list below, and let us know in the comments section which of this year’s posts you liked best!
Continue reading “Five Outstanding Stories From 2022”Empowering Biomedical Research in Rural West Virginia
Public health crises often disproportionately impact rural America. Sally L. Hodder, M.D., works to alleviate these disparities, especially regarding the opioid crisis and the COVID-19 pandemic. She’s the director of the West Virginia Clinical and Translational Science Institute (WVCTSI), the associate vice president of clinical and translational research, and a professor of medicine at West Virginia University.

Dr. Hodder’s work is focused in West Virginia, but her results are valuable assets to researchers across the country. Not only does treating chronic diseases in rural populations contribute to the overall understanding of those diseases, but engaging with and involving people in those communities in research makes science more accessible to them. Dr. Hodder says, “When folks participate in the science, when there is good community discussion about the trial designs and the results, then I think those populations may be more trusting of the results.”
Continue reading “Empowering Biomedical Research in Rural West Virginia”Advancing American Indian and Alaska Native Health Through Research, Training, and Engagement
American Indian and Alaska Native (AI/AN) populations have long experienced health disparities such as higher rates of diabetes, certain cancers, and mental health conditions than those of other Americans. One contributing factor in these disparities is underrepresentation of AI/AN populations in biomedical science—as study participants, researchers, and health professionals. Unfamiliarity with health care options and opportunities, coupled with a distrust of biomedical research resulting from unethical studies in the past, have exacerbated this underrepresentation.
NIGMS-supported researchers, including Native scientists, are partnering with AI/AN Tribes to help reduce health disparities by conducting research focused on AI/AN health priorities and building infrastructure that supports research in those communities. They’re also preparing Native students to pursue careers in science and medicine. In this post, you’ll meet four scientists advancing AI/AN health.
Continue reading “Advancing American Indian and Alaska Native Health Through Research, Training, and Engagement”Science Snippet: Lipids in the Limelight
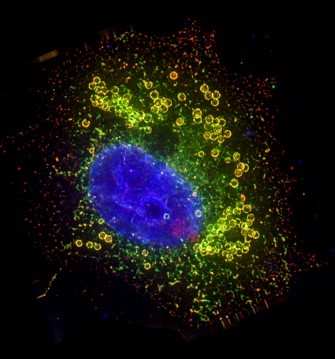
Have you ever wondered why your cells don’t spill into each other or what keeps your skin separate from your blood? The answer to both is lipids—a diverse group of organic compounds that don’t dissolve in water. They’re one of the four major building blocks of our bodies, along with proteins, carbohydrates, and nucleic acids. Types of lipids include:
- Fats, necessary for our bodies’ long-term energy storage and insulation. Some essential vitamins are fat soluble, meaning they must be associated with fat molecules to be effectively absorbed.
- Phospholipids, which make up a large part of cell and organelle membranes.
- Waxes, which help protect delicate surfaces. For instance, earwax protects the skin of the ear canal.
- Steroids, including cholesterol, a precursor to many hormones, which helps maintain the fluidity of cell membranes.
The League of VetaHumanz: Encouraging Kids to Use Their Powers for Good!

“I’m Pink Phoenix, leader of the Vetahumanz League of superheroes, and it’s the best job in the world.” The League of VetaHumanz is a superhero league for veterinarians, founded and led by Pink Phoenix, the alter ego of Sandra San Miguel, D.V.M., Ph.D. Through support from the NIGMS Science Education Partnership Award (SEPA) program, the league seeks to diversify the veterinary profession.
Members of the league work with elementary students across the country to give them a sense of belonging to the veterinary profession. “I’m most proud of bringing people together who share the mission and vision with all their heart,” Pink Phoenix remarks. “Nobody can just be a member of the league. You have to earn the cape.” The league has over 400 certified role models throughout the country who are either veterinarians—VetaHumanz—or veterinary school students—VetaHumanz in training.
Continue reading “The League of VetaHumanz: Encouraging Kids to Use Their Powers for Good!”Public Alerted to Omicron in New Mexico Through Quick Detection
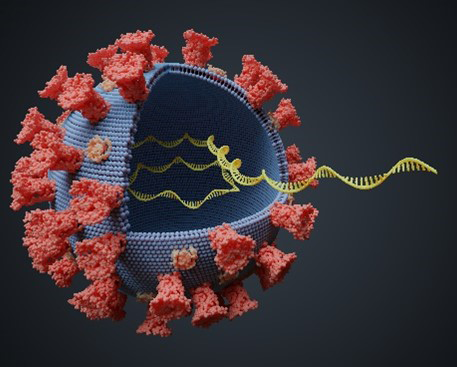
Over the past 2 years, you’ve probably heard a lot about the spread of SARS-CoV-2—the virus that causes COVID-19—and the emergence of variants. The discovery and tracking of these variants is possible thanks to genomic surveillance, a technique that involves sequencing and analyzing the genomes of SARS-CoV-2 virus particles from many COVID-19 patients. Genomic surveillance has not only shed light on how SARS-CoV-2 has evolved and spread, but it has also helped public health officials decide when to introduce measures to help protect people.
In December 2021, the NIGMS-supported SARS-CoV-2 genomic surveillance program at the University of New Mexico Health Science Center (UNM HSC) in Albuquerque detected the first known case of the Omicron variant in the state, which enabled a rapid public health response. The program’s co-leaders, assistant professors Darrell Dinwiddie, Ph.D., and Daryl Domman, Ph.D., were watching on high alert for it to enter New Mexico, and when it did, they were poised to quickly identify it:
Continue reading “Public Alerted to Omicron in New Mexico Through Quick Detection”Researcher Shares Science en Español and Builds a Community

“For me, science is the perfect way to harmonize creative thinking and critical thinking,” says Marcos Ramos-Benítez, Ph.D., a fellow in the NIGMS Postdoctoral Research Associate Training (PRAT) program.
Dr. Ramos-Benítez researches interactions between pathogens—such as the viruses that cause Ebola and COVID-19—and their hosts. He’s also the founder and president of Ciencia en tus Manos (“Science in Your Hands”), a nonprofit organization that presents scientific information in Spanish and aims to provide a community to support the next generation of scientists.
Continue reading “Researcher Shares Science en Español and Builds a Community”Navajo Students Engage With Public Health Research Through NARCH
Navajo students are contributing to public health efforts in diabetes, COVID-19, domestic violence, and maternal and child health through the Navajo Native American Research Center for Health (NARCH) Partnership. “Our goal is to really enhance the educational pathways available to Navajo students from high school to graduate school and beyond,” says Mark Bauer, Ph.D., a co-director of the Navajo NARCH Partnership and professor at Diné College—a tribal college on the Navajo Nation. (Diné means “the people” and is how Navajo people refer to themselves in their native language.)
Continue reading “Navajo Students Engage With Public Health Research Through NARCH”








