
The year 2022 marked 50 years since the creation of the NIGMS Human Genetic Cell Repository (HGCR) at the Coriell Institute for Medical Research in Camden, New Jersey. The NIGMS HGCR consists of cell lines and DNA samples with a focus on those from people with rare, heritable diseases. “Many rare diseases now have treatments because of the samples in the NIGMS HGCR,” says Nahid Turan, Ph.D., Coriell’s chief biobanking officer and co-principal investigator of the NIGMS HGCR. She gives the example of a rare disease advocacy group who worked with the NIGMS HGCR to establish a cell line several decades ago. It was used to identify a gene associated with the disease, which aided in the development of five treatments that have received approval from the Food and Drug Administration.
Researchers have also studied NIGMS HGCR’s samples to help advance knowledge of basic biology and genetics, and even to support the development of a vaccine for a deadly virus.
Continue reading “Propelling Rare Disease Research for More Than 50 Years”







 Dr. Idhaliz Flores-Caldera.
Dr. Idhaliz Flores-Caldera. Sohini Ramachandran, Brown University.
Sohini Ramachandran, Brown University. Credit: iStock.
Credit: iStock.
 Vern Schramm, professor of biochemistry at Albert Einstein College of Medicine, Bronx, New York. Credit: Albert Einstein College of Medicine.
Vern Schramm, professor of biochemistry at Albert Einstein College of Medicine, Bronx, New York. Credit: Albert Einstein College of Medicine.
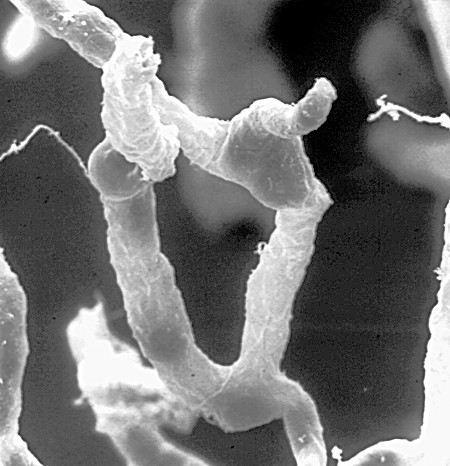 A network of capillaries supplies brain cells with nutrients. Tight seals in their walls keep blood toxins—and many beneficial drugs—out of the brain. Credit: Dan Ferber, PLOS Biol 2007 Jun; (5)6:E169.
A network of capillaries supplies brain cells with nutrients. Tight seals in their walls keep blood toxins—and many beneficial drugs—out of the brain. Credit: Dan Ferber, PLOS Biol 2007 Jun; (5)6:E169.